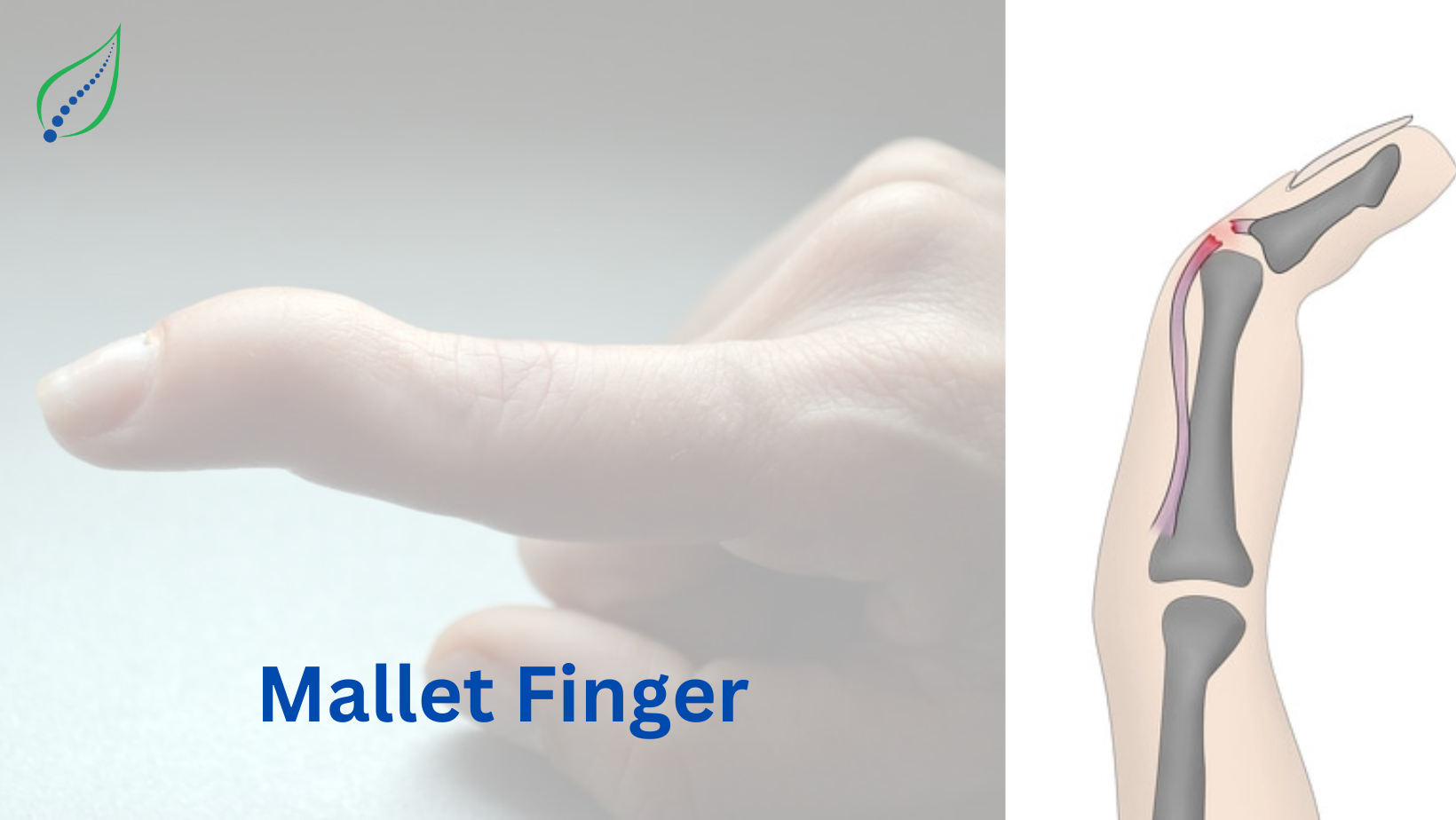
Mallet Finger
Mallet is known as hammer, in finger injuries the distal extensor tendon is damaged therefore the affected finger looks like hammer; it is also known as baseball finger because it is causally seen in sports injuries; In fingers we have 3 small bony joints which are called as phalangeal joints, the proximal joint is called metacarpophalangeal joint (MCP) middle joint is called proximal interphalangeal joint (PIP) and terminal joint is called distal interphalangeal joint (DIP). These joints connect to metacarpal bones which in turn connects to hand bones. These joints sit in volar plates where they are connected by tendons i.e., the strong connective tissue which connects muscle to bone; the tendons are attached to MCP, PIP, DIP joints but their muscles are located in forearm region. The tendons which connect to DIP joints are extensor tendons with action of extension of digits vice versa there are flexor tendons on palmar side which help in bending digits. The mallet finger injuries occur due to disruption of extensor tendons. The sequence of common mallet finger injuries is middle finger >ring finger > index finger> little finger than thumb.
CAUSES:
- Forced violent flexion
- Laceration of dorsum of finger at DIP
- Finger stucked at DIP end resulting tear or disruption of extensor tendon
Disruption of extensor tendon causes DIP to droop or fixed in flexion position with loss of ability to extend the joint resulting flexion deformity like hammer.
Doyle’s mallet finger classification:
It has 4 categories:
- Closed with or without avulsion fracture
- Open laceration with discontinuity of tendon
- Deep abrasion with skin loss and loss of tendon continuity
The fourth category includes another 3 sub types:
- Trans epiphyseal plate fracture in children
- fracture of articular surface between 20-50%
- Fracture of articular surface > 50%
SYMPTOMS:
- Pain and swelling over end of finger
- DIP joint flexed or in bent position
- Inability to hold finger straight at DIP joint
- Restricted active range of motion
DIAGNOSIS:
Radiographs with Anterior - posterior, lateral, oblique view centered at DIP joint of the affected finger shows the mallet finger categories.
TREATMENT:
Soft tissue mallet finger- this type of mallet finger conditions where there is no fracture only soft tissue damage present and these are treated with splint which are highly effective.
Other splinting techniques include Stack splint, aluminum foam splint, perforated splints are more beneficial than solid splints.
The splinting duration is 6-8 weeks and progressive flexion exercises are started at 6 weeks. It should be encouraged to keep the splint on at all times as removal and flexion of the joint reset the 6-to-8-week clock back to time zero.